RA – A Double Edged Sword
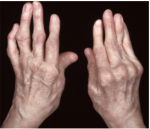
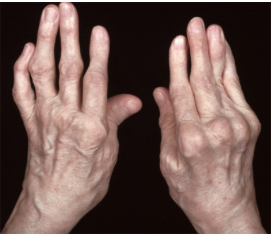 Rheumatoid arthritis (RA) is a chronic systemic autoimmune disease that causes progressive pain, inflammation and eventual destruction of the joints.
Rheumatoid arthritis (RA) is a chronic systemic autoimmune disease that causes progressive pain, inflammation and eventual destruction of the joints.
RA can occur at any age, but usually appears between the ages of 35 to 64. It is the second most common form of arthritis (after osteoarthritis) affecting nearly half a million Australians (2% of the population). An estimated 57% of people with RA are women.
RA is relatively rare in Indigenous Australians compared to non-Indigenous Australians. It is believed that this is due to a lack of genetic factors that predispose a person to this autoimmune disease.
At its worse RA reduces a person’s capacity to work, with only 31% of those affected in fulltime employment compared with 53% of the general population
The hallmark feature of this condition is long term inflammation of joints that is mirrored on the opposite joint. It affects the hands, wrists and feet, although any joint lined by a synovial membrane may be involved.
RA is a Systemic Disease
- Skin
- Eyes and Mouth
- Nervous System
- Lung
- Heart
- Blood Supply
The Immune System Views Synovial Fluid as an Invader
The immune system views the synovial fluid in joints as foreign invaders and attacks the synovium. The resulting inflammation thickens the synovium (called pannus formation), which can eventually destroy the cartilage and bone within the joint.
Inflammation causes the joints to become painful, hot and swollen and movement is restricted. Stiffness in the joints is common, especially in the morning. The inflammation caused by RA can result in permanent damage to the joints particularly if left untreated.
Three Possible Clinical Courses of RA
Course I: Monocyclic
About one-third of those who get RA will have complete remission within 2 years of the disease onset.
Course II: Polycyclic
This is most common course, affecting around 40% of people with RA. It is characterised as being slowly progressive punctuated by flare-ups (acute activity) and remissions. Flare-up periods last longer over time.
Course III: Progressive
This aggressive course occurs in almost 20% of RA cases. This course is the most constant and destructive form of the disease which causes deformity, disfigurement and even premature death.
Symptoms of RA
Symmetrical (both) hand effects are the most prominent feature of RA.
The most common symptoms of RA include:
- Swelling, pain and heat in the joints, usually the smaller joints affecting the hands or feet
- Stiffness in the joints, especially in the morning
- Persistent fatigue
- Limited movement of the affected joints
- Sleeping difficulties because of the pain
- Weak muscles
A joint is where two bones meet to allow movement and flexibility. This movement is controlled by muscles attached to the bone through tendons. The ends of the bones within a joint are covered by a smooth tissue called cartilage, which enables one surface to glide over the other.
Each joint is surrounded by a capsule that protects and supports it. The capsule is lined with synovium, a type of tissue that produces fluid to lubricate and nourish joint tissues.
In a healthy joint, this lining is very thin, has very few blood vessels in it and does not contain any white blood cells.
In cases of RA the immune system initially attacks the synovium. White blood cells move from the blood stream and invade the synovium and small blood vessels also infiltrate the area. As a result the synovial membrane becomes thick and inflammed, resulting in unwanted tissue growth. The inflammation also involves the release of various biochemical substances causing pain, swelling and joint damage.
These substances eventually damage the surrounding cartilage, bone, tendons and ligaments. When these substances enter the bloodstream, they can cause fatigue and a general feeling of being unwell.
Over time the joint irreversibly loses its shape and alignment.
Causes of RA
Auto Immune Disease
The immune system targets the lining of the joints (the synovial membrane) causing inflammation and joint damage. The characteristic swelling found in RA occurs when the joint produces too much synovial fluid in response to the inflammation. Being a systemic disease, other parts of the body such as the lungs and eyes may also be affected.
Genetic Factors
Persons with RA often have family members or close relatives with the disease. If one member of a family has RA then other family members are three or four times as likely to develop the disease as the general population. It is believed that the HLA (human leukocyte antigens) genes are associated with a variety of autoimmune processes including RA.
Hormones
Sex hormones may play a role in RA, as evidenced by the larger percentage of females with this disease, its improvement during pregnancy, its recurrence in the early postpartum period, and its reduced incidence in women using oral contraceptives.
Hyperprolactinaemia (high levels of prolactin) may also be a risk factor for RA.
Infections
Numerous infections have been suggested as possible causes for RA, including Mycoplasma organisms, Epstein-Barr virus, rubella and gingivitis bacteria.
Lifestyle
Smoking increases the risk of developing RA especially in those people who are genetically predisposed.
Environment
Various environmental factors have been identified as potential risk factors for RA development including the gut microbiota, vitamin D deficiency, silica dust exposure and mineral oils.
Early diagnosis and intervention are critical to improving the outcome of RA. Studies show that people who receive early treatment for RA feel better sooner and more often, and are more likely to lead an active life. They also are less likely to have the type of joint damage that leads to joint replacement.
Diagnosis of RA depends on the symptoms and results of a physical exam – including warmth, swelling and pain in the joints.
Some blood tests also can help confirm RA.
Telltale pathology includes:
- Anaemia (a low red blood cell count)
- Rheumatoid Factor (RF). This is an antibody (blood protein) found in about 80% of patients with RA over time, but in as few as 30% at the onset of the disease. Somewhat confusingly about 5% of people without the disease test positive.
- Antibodies to cyclic citrullinated peptides (pieces of proteins), or anti-CCP for short (found in 60–70% of patients with RA)
- Elevated erythrocyte sedimentation rate (ESR). This is a blood test that, in most patients with RA, confirms the amount of inflammation in the joints)
X-rays can help in detecting RA, but may not show anything abnormal in the initial stages of the disease. However these first X-rays may be useful later to show if the disease is progressing. Often, MRI and ultrasound scanning are done to help judge the severity of RA.
Orthodox Medications Commonly Prescribed
A number of orthodox medications are commonly prescribed (usually in combination) to people with RA.
These include:
- Disease modifying anti rheumatic drugs (DMARDs)
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Corticosteroids
- Biologic Agents.
All have considerable side effects.
Disease modifying anti rheumatic drugs (DMARDs)
- Methotrexate (e.g. Methoblastin) is the most commonly used DMARD. It can be administered either orally or intramuscularly. Supplements of folic acid are required to help minimise side effects such as nausea and mouth ulcers. Methotrexate is potentially toxic to the liver and alcohol consumption should be avoided if taking it.
- Sulfasalazine (Pyralin EN and Salazopyrin) is used to treat mild RA. It is less potent than some other DMARDs. It can cause nausea, dyspepsia, diarrhoea, rash and headaches. More seriously, it can cause severe anaemia.
- Leflunomide (Arabloc and Arava) is used to treat severe active RA that does not respond to classical DMARDs such as methotrexate.
- Intramuscular gold injections of sodium aurothiomalate (Myocrisin) is rarely used. Side effects of gold injections include mouth ulcers, rash, thrombocytopenia (a deficiency of platelets — cells that are involved in blood clotting) and proteinuria (protein in the urine).
- Oral gold such as auranofin (Ridaura) is also rarely used, largely because of poor efficacy. Diarrhoea is a common side effect.
- Antimalarials such as hydroxychloroquine sulfate (Plaquenil) are used in the treatment of mild RA. Hydroxychloroquine is often used in combination with other DMARDs. Adverse effects include retinal toxicity. A person is required to see an eye specialist periodically if taking this medicine.
- Cyclosporin (Cicloral, Neoral and Sandimmun), originally developed to prevent organ rejection in transplant patients, is used either on its own or in combination with other anti-arthritic drugs. It produces many adverse effects, including hypertension (high blood pressure) and impaired renal (kidney) function.
- Azathioprine (e.g. Imuran) is limited to the treatment of severe active RA that is unresponsive to other DMARDs and to treat people with rheumatoid vasculitis (a serious complication of severe RA in which blood vessels are inflammed). Because of high toxicity it is now seldom used.
Often, doctors prescribe DMARDs along with NSAIDs and/or low-dose corticosteroids in an attempt to lower swelling, pain and fever.
Non-steroidal anti-inflammatory drugs (NSAIDs)
NSAIDs are commonly prescribed to reduce pain and inflammation. They do not stop the disease from progressing.
Ibuprofen (e.g. Nurofen) and naproxen sodium (e.g. Naprogesic), are available over the counter,
Diclofenac (e.g. Voltaren), piroxicam (e.g. Feldene), sulindac (Aclin) and indomethacin (e.g. Indocid), are available as prescription medicines only.
The use of NSAIDs is often limited because they increase the risk of upper gastrointestinal problems, such as gastric ulcer. They are not suitable for use by people who have had a peptic ulcer or gastrointestinal bleeding.
- COX-2 specific inhibitors
The coxibs (e.g. celecoxib — brand name Celebrex) are non-steroidal anti-inflammatory agents. Studies have shown that the coxibs have lower rates of gastric ulcer associated with them than the conventional, older NSAIDs.
However Coxibs are associated with an increased risk of cardiovascular events, such as heart attack and stroke, when taken in high doses. People who have an increased risk of heart attack or stroke should not take these medicines.
Corticosteroids
Corticosteroids, sometimes known as glucocorticoids, such as prednisone (e.g. Panafcort) and prednisolone (e.g. Panafcortelone), work by reducing inflammation and suppressing the immune system. They are used in the treatment of RA, both as tablets and as injections into the joint.
Prednisolone is sometimes prescribed by GP’s for moderate to severe RA when NSAIDs and DMARDs have not had the desired outcome. Oral corticosteroids are usually used at the lowest effective dose but still have adverse effects such as weight gain, hypertension and osteoporosis.
Corticosteroids may be injected into the joints if the arthritis is not being controlled by oral therapy, but this should be limited to 3 to 4 injections a year. Joints commonly injected are fingers, toes, knees and shoulders. Corticosteroids are also sometimes injected into the muscles or given via an intravenous infusion.
Biologic agents
TNF inhibitors
A category of arthritis treatments called biologics has been recently developed. The most notable is the tumour necrosis factor (TNF) inhibitors. TNF occurs naturally in the body and is a key player in the inflammatory process in RA. It is found in high concentrations in the joint fluid of people with RA. By attaching to the TNF molecule or its receptors on cells, these new agents can block its effect.
- Infliximab (Remicade) slows the progression of RA and reduces joint damage. It is given by infusion via a drip into a vein. Each treatment takes approximately 2 hours. Infliximab is given in combination with methotrexate. In Australia there are very tight Government restrictions on which patients with RA can be treated with infliximab.
- Etanercept (Enbrel) is used for the treatment of active RA in adults who have had an inadequate response to several DMARDs, including methotrexate. It is given by injection under the skin once or twice weekly.
- Adalimumab (Humira) is the third TNF inhibitor that has been added to the list of approved agents for RA. It is administered by injection under the skin, once a fortnight.
They can only be prescribed by certain medical specialists (rheumatologists and clinical immunologists).
Studies to evaluate the long-term safety of these powerful and expensive agents, have found in addition to some other side effects, an increased susceptibility to infection in people taking these medicines.
Newer biologic agents
Over the past few years several new biologic agents have been developed which target substances in the body other than TNF.
- Rituximab (Mabthera) is a monoclonal antibody targeted against certain white blood cells called B lymphocytes. (Monoclonal antibodies are proteins that are produced in the laboratory to recognise and bind to proteins found in the body.) It is given as 2 intravenous infusions 2 weeks apart.
- Abatacept (Orencia) is another monoclonal antibody targeted at specific molecules found on cells called T lymphocytes. It is given as a monthly intravenous infusion.
- Anakinra (Kineret) is called an interleukin-1 antagonist. It blocks the action of interleukin-1, a protein present in the body that is produced in high concentrations in people with RA. Anakinra is given by injection under the skin.
RA’s Impact
RA can have a dramatic impact on both metal health and daily living for individuals.
Mental health
The mental health of people with RA can be severely affected by the chronic pain and ongoing physical disability. The constraints imposed by the disease can be detrimental to a person’s self-esteem and self-image. People with the disease can suffer from depression, anxiety and feelings of helplessness.
Daily Living
Disability caused by RA can make daily living activities difficult to do. Physical limitations and a lack of energy may affect normal household chores, caring or a family or even oneself. Mobility can be particularly limited and may restrict participating in social activities and employment. Social interactions may become difficult soon after initial diagnosis because of the rapid, early deterioration in physical abilities.
For persons aged 15–64 years, being unable to work is one of the most common problems associated with RA. The inability to work causes major financial and psychological issues for both individuals and their family. There is also the social and economic burden placed on the community resulting from a person’s incapacity to maintain employment.
Natural Therapies Can Help Alleviate the Symptoms of RA
There is no ‘one size fits all’ treatment protocol for RA as its course and severity varies from person to person and no two cases are the same.
RA symptoms may change from day to day where there are alternating active and ‘flared’ up days and at other times when it is inactive and good days.
Fish Oil
Studies of RA patients showed they had less inflammation (and pain) and were able to reduce their NSAID medication when taking fish oil. In addition, the consumption of fish oils may help safeguard against cardiovascular disease, a condition commonly associated with RA.
Evening Primrose Oil (EPO) or Borage Oil
Supplementing with gamma-linolenic acid (GLA), an essential omega-6 fatty acid found in vegetable oils such as evening primrose, blackcurrant or borage seed oils is known to relieve pain, morning stiffness and joint tenderness in RA patients.
Selenium
People with RA have been found to have lower selenium levels than healthy people. A double-blind trial using at least 200mcg of selenium per day for 3-6 months found that selenium supplementation led to a significant reduction in pain and joint inflammation in RA patients.
Taking selenium improved joint swelling, tenderness, and morning stiffness, as well as reduced the need for supplemental cortisone and non-steroidal anti-inflammatories for symptom control.
Vitamin A
Vitamin A has been recently shown to control chronic immune mediated auto immune inflammatory diseases such as RA by influencing inflammatory markers.
Hemidesmus
The herb Hemidesmus has been shown to suppress both the cell-mediated and humoral components of the immune system which is of benefit in autoimmune disorders such as RA.
Research has also demonstrated that Hemidesmus has anti-arthritic activity comparable anti-arthritic activity of methotrexates. This suggests that hemidesmus has protective activity against arthritis.
Berberine
One of the main active constituents in the herb phellodendron is berberine (BBR). BBR has been shown to exert immunosuppressive and anti-inflammatory effects in several autoimmune diseases including RA by reversing pathological changes and reducing inflammation.
Vitamin D
A study has determined that Vitamin D in RA patients was significantly lower than that in the controls being deficient in 50.8%, insufficient in 23.8% and normal in 25.4%.
Vitamin D deficiency is strongly associated with musculoskeletal problems and autoimmune and inflammatory diseases such as RA. If levels are below 80nmol/L, 5000IU is recommended per day. Once vitamin D levels have normalised a maintenance dose of 2000IU/ day can be taken.
This indicates that vitamin D may play as an immune modulating agent to suppress inflammation and therefore reduce pain.
Lifestyle Modifications
- Perform low-impact aerobic exercises, such as walking, and exercises to boost muscle strength. This will improve overall health and reduce pressure on the joints.
- Maintain a positive attitude in self-managing the disease. Research has shown that people who take control of their treatment and are active in managing their disease experience less pain and make fewer visits to the doctor as they have a better strategy at managing their own mental health.
- Weight control. Excess weight puts added stress on joints in the body and can also make joint surgery, if required, more difficult.
- Dietary variation. Although research has not identified a specific diet to treat RA, there is discussion surrounding various types of diets. Some people may benefit from following a vegetarian or Mediterranean diet, or by avoiding foods that make their condition worse. These include pro-inflammatory foods such as wheat and refined grains – ie. biscuits, white breads and pastas, excess caffeine, alcohol and fried foods as they contribute to inflammation, low energy and poor immune health.
- Heat application. The application of heat can help ease pain, relax tense, painful muscles and increase blood flow. Heat is particularly helpful if used before exercise, but should not be used on joints that are already hot and swollen.
- Cold application. Applying cold treatments to joints that are hot and swollen can help manage acute symptoms.
- Use of assistive devices. Many devices are available to help people with RA manage their everyday activities. For example, walking canes, braces for painful joints and jar grippers can assist with daily living.
- Rest. Sufficient rest is an important component of disease management that can help improve symptoms when joints are inflammed and painful.
Further Reading
- Acid/Alkaline and pH Balancing
- Are Grains The Cause of Your Pain?
- How Diet Can Feed Inflammation
- Sunlight Vitamin Holds The Key To Autoimmune Disease
- Nurofen, Stomach Ulcers and Bleeding from the Bowel
- Is Pain Relief Worth Dying For? Voltaren Increases Stroke Risk By 63%
- The Mediterranean Diet: The World’s Healthiest Diet?
- Arthritis – Osteoarthritis
The Spinal Centre – Neuro-Musculoskeletal SolutionsThe Spinal Centre provides the Best Natural Medicines, Health Products and Nutritional Solutions to Free You of Pain and Improve Your Spinal Health.The Spinal Centre is a leader in the management and treatment of spinal pain and disability including:
- Chronic Back and Neck Pain
- Cervical and Lumbar Disc Injuries with or without neruological changes
- All forms of arthritis including rheumatoid arthritis, psoriatic arthritis and osteoarthritis
- Neurodegenerative diseases such as Parkinson’s and Alzheimer’s disease
- Neuromuscular problems such as chronic back pain, headaches, migraines, neck or spinal pains
- Myofascial pain syndromes such as fibromyalgia, diffuse muscular or joint pains
- Austistic spectrum disorders including ADD, ADHD, learning difficulties and autism
- Fatigue, energy and mood disorders including chronic fatigue and depression
The Spinal Centre focuses on resolution with the development of individualised treatment programs using Conservative and Integrative Medicine; combining genetic, metabolic and nutritional testing with specific natural medicines to enhance your health and achieve your genetic potential.We have helped thousands – Why Not You?